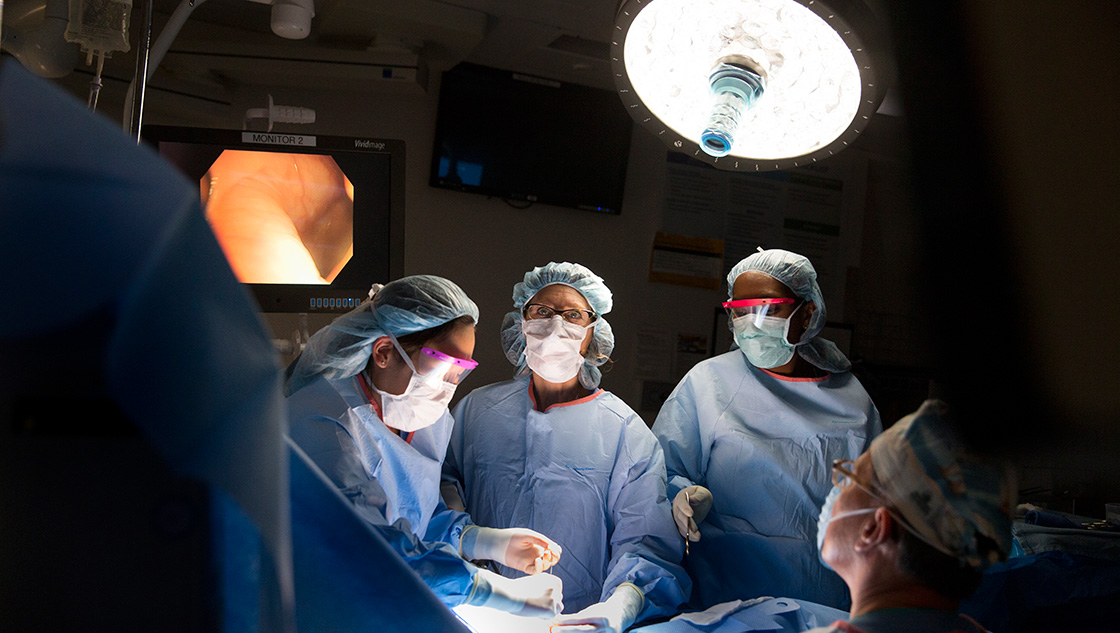
Photos by Rose Lincoln/Harvard Staff Photographer
Leaving a beautiful scar
With note-perfect poise, Terry Buchmiller cares for the tiniest of patients
Windsurfer Gonzalo Giribet and pianist Vijay Iyer have also been featured in Practice, a series of profiles zeroing in on the makings of performance.
A surgeon’s knot seems a simple thing, tied to keep the insides in and the outside out.
But a simple knot can be harder — and more vital — than it looks. A surgeon tying a knot isn’t like the rest of us tying our shoes, unless you sometimes tie with one hand or clutch your laces with surgical instruments.
For physicians who’ve delved into the mysteries of loops, throws, and ears, square knots are routine and, with an extra overhand turn, become surgeon’s knots, less likely to slip. Only when they’re mastered can they be used in procedures, where knowledge of anatomy and disease are also crucial, where a knot too loose can cause a wound to leak and one too tight can kill the tissue it encircles.
“I learned by practicing constantly as a medical student,” said Terry Buchmiller, an assistant professor of surgery at Harvard Medical School and Harvard-affiliated Boston Children’s Hospital. “The nurses would let us take the extra suture that wasn’t used during an operation. They’d always slide it to the medical student so we could grab it and go back and just sit and doodle [with it] and tie knots at home.”
By now, the many steps behind a successful surgery — including knot-tying — are mostly second nature to Buchmiller, who specializes in the delicate work required on small children, newborns, and, when necessary, fetuses in the womb.
But in the beginning, surgery was exactly as music had been.
Growing up in Cupertino, Calif., Buchmiller first picked up the violin at 7, spending hour upon hour practicing the scales and finger positions. By high school she’d performed in two symphonies. She was a music major in college, practicing five or six hours a day to master a piece: the perfect placement of her fingers, the just-so angle of the bow, the bouncing arpeggio stroke, the tremolo’s fluttering repetition. As a member of the Longwood Symphony Orchestra, the memory of those sessions is more a feature of action than reflection.
“At one point, in high school, I played three to four to five hours a day; during college, as a music performance major, sometimes five to six hours a day. So it was a tremendous amount of focus on that skill.”
But it was a focus held in balance. Buchmiller had taken up her pediatrician on his offer to follow him around and observe his work. She was 15 when she saw her first surgery, at the University of California at San Francisco. She was always fascinated by the ability to fix what ailed people.
“That interest never waned,” Buchmiller said. “I never had to decide what to do when I grew up.”
‘You walk in and there’s a performance, that one-time performance for that patient.’
Though the two may seem opposites, medicine and music have pulled her along instead of apart, Buchmiller said. The way of practice taught to her by music was mirrored in medicine: Break the complex down to its composite parts, learn those parts through intense practice, and then put them together into a greater whole.
“The traditional way surgery and music is taught, the way that I learned both, was to focus on the individual building blocks, each individual skill, and then learn the big picture. Very scientific and very logical at the beginning and putting in the emotional part and the nuances only when your fingers know what to do, when your hands know what to do.”
Even after years of performing general surgery, there was still plenty to learn, as Buchmiller realized when she arrived at Children’s Hospital in 1995 to begin her fellowship in pediatric surgery.
“I could tie knots perfectly for a general surgeon, but now let’s try some on a baby. You’ve been through nine years of general surgery training and then you were told … well, that you had an opportunity to learn to be gentle all over again. That philosophy — because we do work on babies and children — that delicacy is paramount is something that is still ingrained in my head. Every time I go into the operating room, I still hear that voice from my mentor, and maintain a critical eye for not only my fellows’ and my residents’ hands, but mine as well.”
But medicine is more than craft. The surgical skills that seem important to her today aren’t physical tricks or manipulations of the scalpel, but qualities of mind: focus and teamwork.
“I think one is stamina. There’s no question that the ability to stay focused is a huge piece of surgery. This intense focus — I mean, hours can go by. Music may not [require] the same stamina, musical concerts are usually for a finite time, but I think the team-building skills are fairly similar.
“Whether or not you’re the head of a surgical team in the operating room or if it’s just you and a pianist, or you as part of a symphony orchestra, it’s a team.”
An operation requires a unit just as a symphony requires individual musicians. Each individual has to master specific skills, whether it’s administering anesthesia or playing certain notes, for the group to realize its goal.
“If you really look at the way a conductor rehearses a symphony, they break the parts down and they drill [musicians] in the parts and then, only when we know the mechanics of it, can the conductor really be free to put the whole together to make the music, interpret the music,” Buchmiller said.
“Our conductor’s always trying to embed in our … heads, ‘Please don’t wait until the last week to learn the notes because I want to make the music and I can’t make the music until you all really know the notes.’”

Then there are the notes of the operating room, individual acts by doctors and nurses and even by increasingly sophisticated machines, beeping and whooshing and tracing bright lines. These notes, punctuated, if all goes well, by the perfect knot, will never be played in quite the same way again, but the patient will live with them forever.
“You walk in and there’s a performance, that one-time performance for that patient,” Buchmiller said. “You want the scar to be beautiful, because the kids are going to have that for, God willing, 70 or 80 years.”





