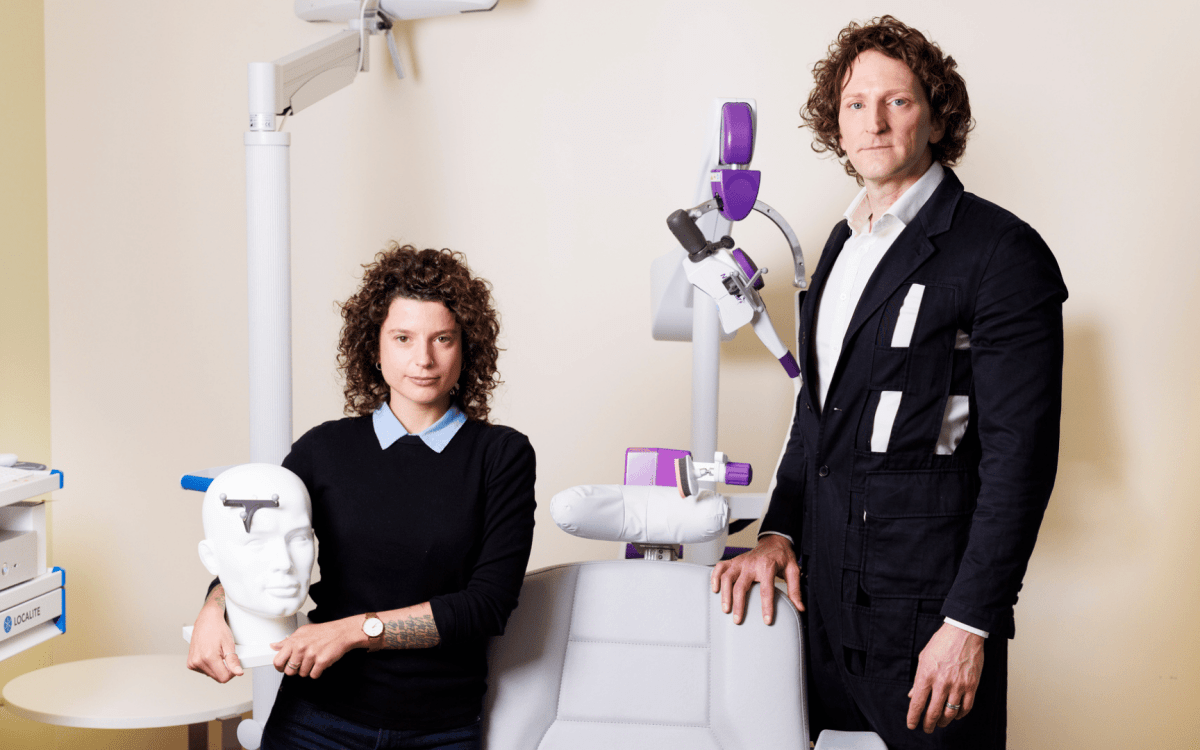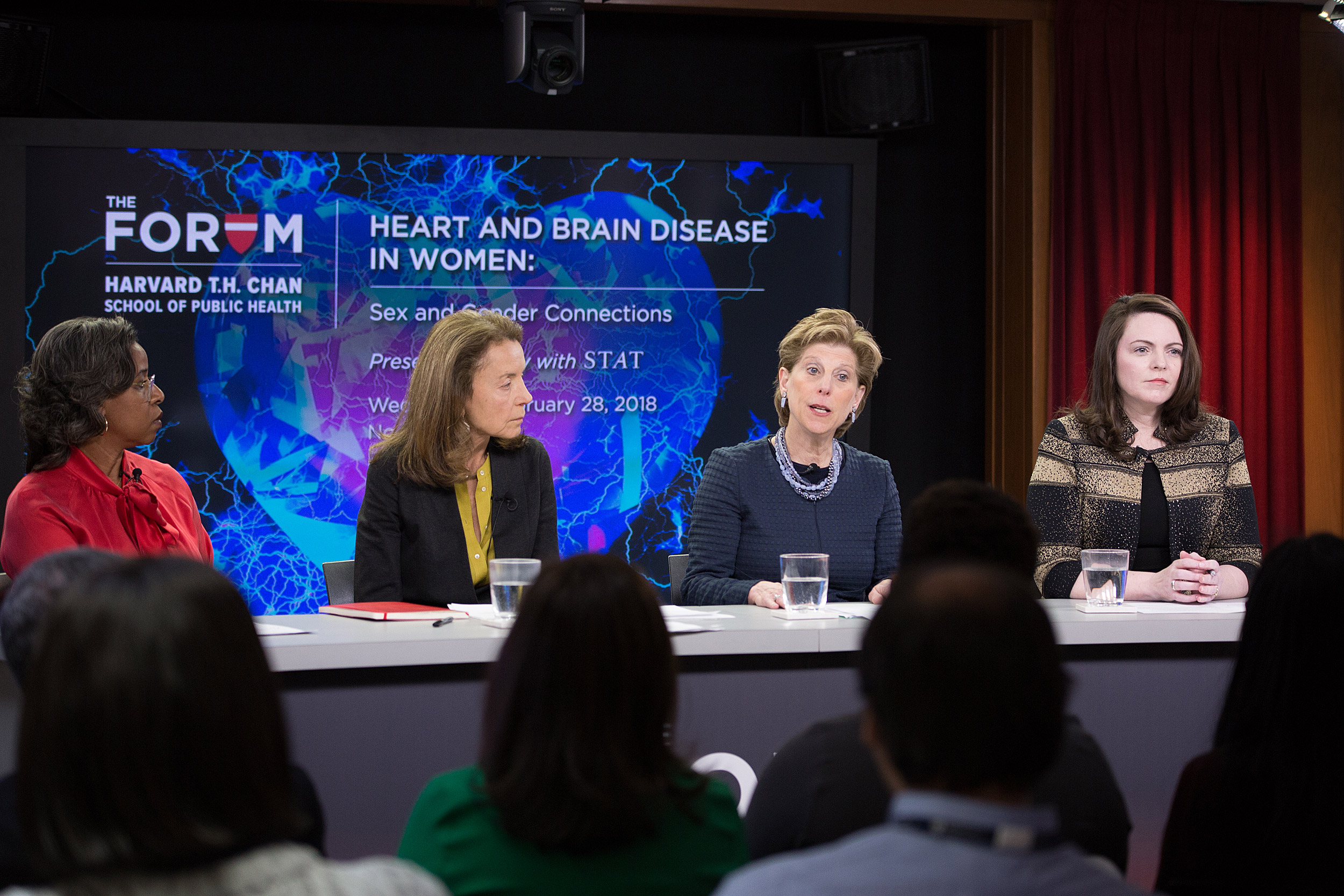
Despite progress in recognizing and incorporating sex-based differences in the health of men and women, work remains, contend panelists British Robinson, Ana Langer, Jill Goldstein, Marjorie Jenkins, with moderator Sharon Begley.
Sarah Sholes/Harvard Chan School
When disease strikes, gender matters
Experts in Harvard Chan School discussion say research, treatment need to be more sensitive to differences between men and women
Much of how we attack serious illnesses like heart disease, depression, and Alzheimer’s has been informed by studies of men. And that approach misses important differences between men and women in how the diseases look, progress, and respond to treatment, according to panelists at the Harvard T.H. Chan School of Public Health.
“[We need] education and awareness on every level, with every sector,” said British Robinson, chief executive officer of the Women’s Heart Alliance. “We have to take a whole-systems approach. That system includes our medical and clinical systems, hospitals systems. It includes our physicians, our nurses, our community health workers.”
Differences between men and women are particularly salient in diseases of the heart and brain, panelists said, including heart attack and heart failure, major depression — which occurs at double the rate in women — and Alzheimer’s disease, which strikes women more frequently than their longer average lifespans explain.
More women experience heart attacks that have atypical symptoms, including heartburn, back pain, anxiousness, and fatigue. In addition, women tend toward smoother arterial plaque, which can make heart disease harder to diagnose through catheterization, panelists said.
“They’re called ‘atypical’ because the ‘typical’ was defined on the male norm, and so when women present with burning or back pain or jaw pain they’re often triaged in a different way in the emergency room,” said Marjorie Jenkins, director of medical initiatives and scientific engagement for the Food and Drug Administration’s Office of Women’s Health. “So a woman comes in. She’s anxious. She has heartburn. She has back pain. She’s questioned. She tells the doctor she’s tired. She’s really nervous. So the doctor thinks she’s having a panic attack or she’s depressed and therefore she gets medication for that. Those medications will not treat a heart attack. She needs to be screened for heart disease.”
Harvard Medical School Professor of Psychiatry and Medicine Jill Goldstein, who heads the Women, Heart and Brain Global Initiative at Massachusetts General Hospital, and Ana Langer, a professor of the practice of public health and director of the Women and Health Initiative at Harvard Chan School, also participated in the discussion on Wednesday, “Heart and Brain Disease in Women: Sex and Gender Connections.”
One opportunity for raising awareness is in research, panelists said, noting that before recent gains, women were underrepresented for decades. Even when women are included, data isn’t always analyzed by sex, missing an opportunity to tease out gender differences.
“If we don’t get the data, we won’t know the answers,” Jenkins said.
To truly understand gender disparities, researchers should design trials in a way that accounts for factors such as the natural ebb and flow of hormones, which Goldstein cited as a possible driver of differences. Studies also need to account for the influence of life stages such as puberty, pregnancy, and menopause, panelists said.
The Food and Drug Administration has for years required new drug applications to include analysis of data by sex, Jenkins said, and the National Institutes of Health enacted a policy in 2016 that required research funded by NIH grants to consider the role of sex as a biological variable. Jenkins said that studies should also examine differences in age and racial and ethnic backgrounds to capture the true diversity that exists in the population.
“We need women of color, we need women of different backgrounds, we need women of different ages,” Jenkins said. “We need to need to know those answers for all women, and all men. So that’s why very it’s important to participate so we can have those answers and treat patients to the highest level of care.”
The problem is not restricted to the U.S., Langer noted. Women in developing nations face particular challenges because rates of smoking and obesity are increasing while health care systems are often weak.
Looking ahead, Goldstein urged that precision medicine, in which treatment is tailored to individual needs, aim for inclusiveness in clinical trials, analysis of results by sex, and heightened awareness among doctors and nurses of sex-based differences.
“[It’s important to be] educating the next generation who are going into medicine and educating the public about the importance of the impact of sex on what we now are terming personalized, individualized, precision medicine,” Goldstein said. “Because … what could be more personal than one’s sex?”