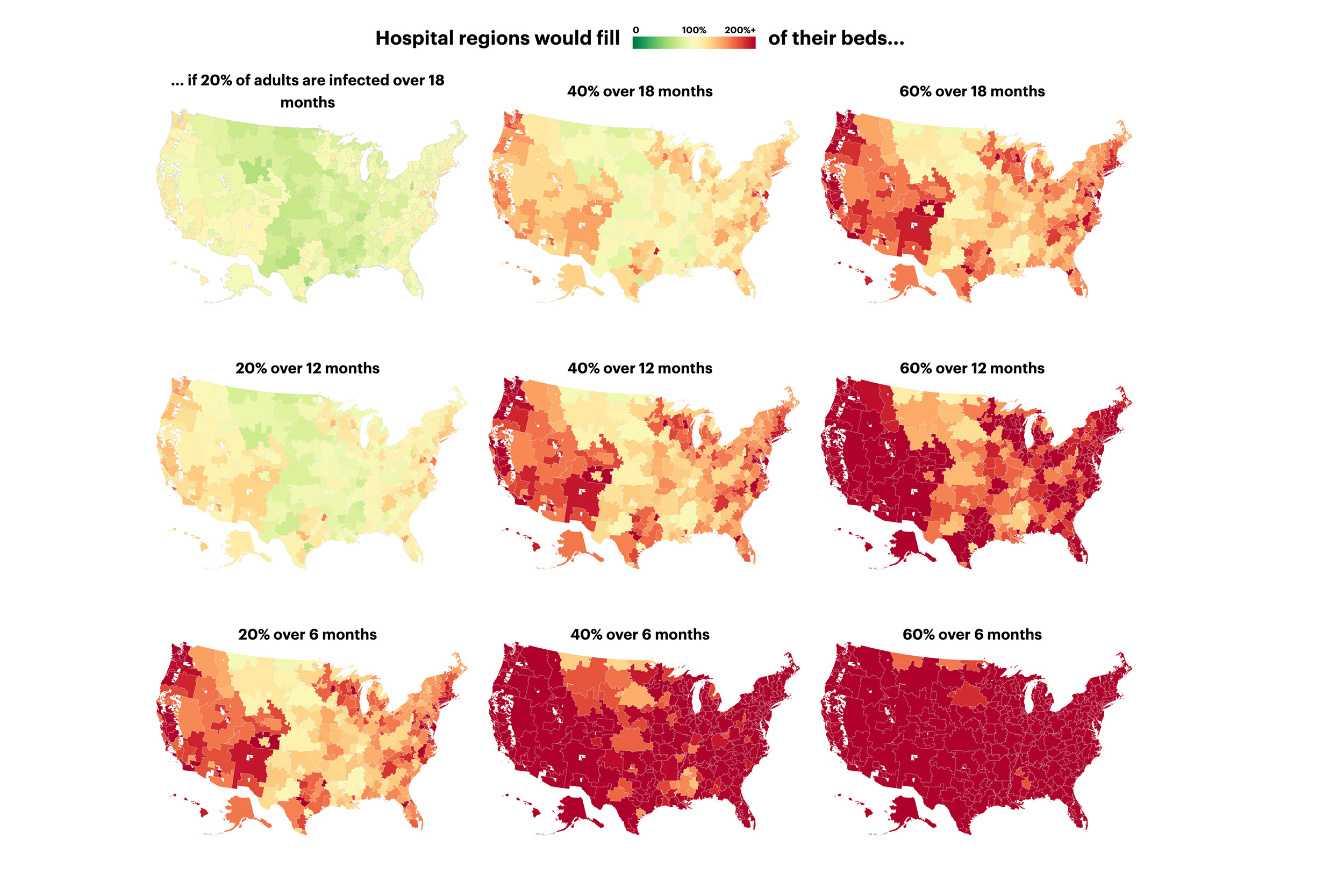
In this screen shot, every hospital referral region (HRR) in the U.S. is shown under different scenarios, colored by whether it would be over capacity or not. Top-left: capacity for 20 percent over 18 months. Bottom right: 60 percent over six months. The data is from the model developed by Harvard Global Health Institute researchers, as shown in an app developed by ProPublica.
Source: Harvard Global Health Institute, Hospital Bed Capacity & COVID Estimates
App predicts hospital capacity
New tool will help leaders make informed decisions as hospitals prepare for COVID-19 patients
This is part of our Coronavirus Update series in which Harvard specialists in epidemiology, infectious disease, economics, politics, and other disciplines offer insights into what the latest developments in the COVID-19 outbreak may bring.
An interactive tool that compares hospital-care capacity with projected demand in the nation’s 306 hospital referral regions was launched Tuesday by the Harvard Global Health Institute (HGHI), in collaboration with ProPublica. It shows specific gaps to address at the local level, helping policymakers and hospital leaders prepare for an influx of COVID-19 patients.
HGHI has research teams that study health care capacity and quality throughout the world. As the number of coronavirus (SARS-CoV-2) infections began to rise in the U.S., one group put their machinery into motion to empower local leadership to plan according to need.
“Last week we started seeing what was happening in northern Italy, with hospitals overwhelmed by COVID-19 patients. Since northern Italy has more hospital beds per capita than the U.S., we realized that we’d have the same problem here — but we didn’t have the data people need to make decisions on the ground. We started working on it right away, getting up-to-date information at the local community level because that’s what governors, mayors, and hospital executives need,” said HGHI Director Ashish Jha, K.T. Li Professor of Global Health at Harvard.
“Three weeks ago, we were getting increasingly frustrated as we watched the U.S. miss the boat on testing,” said Thomas Tsai, part of the research team that developed the model. “But the minute we realized we were in mitigation mode, we put our machinery in motion to help hospitals get in a better position to prepare. Now, we’re providing data do that hospital leaders and policymakers can see clearly, right now, the degree of the capacity gap. Then they can look at postponing elective surgeries and taking other measures to increase capacity.”
Tsai is an assistant professor at the Harvard T.H. Chan School of Public Health and the Global Health Institute, and a surgeon at Brigham and Women’s Hospital.

“… We hope this project will help change the national conversation from panic to planning,” said Ashish Jha, director of the Harvard Global Health Institute.
Courtesy of HGHI
The launch coincided with reports about the data in The New York Times and CBS Morning News. The new model is based on the American Hospital Directory and the American Hospital Association database: the most comprehensive annual survey of hospitals in the country. Information about current and projected inpatient and ICU bed availability, equipment, and professional capacity is mapped to age and other data from the U.S. Census, then adjusted for population size, age distribution, projected hospitalization rate, and other factors.
“Our goal was to provide actionable information for hospital leaders across regions, states, and at a national level so they can truly understand the gap between available beds and potential demand,” said Tsai. “That way, we’re less likely to be stuck in a situation where physicians are faced with an onslaught of patients and forced to make difficult choices about rationing ventilators and beds. We’re providing information that helps hospital leaders make the tough choices before the wave hits.”
A new app developed by ProPublica gives a clear picture of best- and worst-case capacity scenarios by region. It reflects variables such as number of beds available, ICU capacity, population over 65, and projected infection rates (20 percent, 40 percent, 70 percent). By visualizing scenarios for different time frames (six months, 12 months, 18 months), decision-makers can see where communities need to focus to ensure they have enough hospital beds, trained professionals, and equipment.
More like this
The data show a profound mismatch in most U.S. markets between available bed supply and the projected demand for inpatient and ICU beds for COVID-19 patients. With most hospital beds occupied in any given market (as a matter of business practice), HGHI researchers say the number of ICU beds is below what would be needed to meet full demand if the coronavirus disease runs its course.
One measure that hospitals can take is canceling elective surgeries, which would free up inpatient beds, decrease the chance of transmission, and ease a bottleneck in the availability of ventilators. Creating that capacity is essential so that patients with cancer, complications of pregnancy, and traumatic injury can continue to get the high-quality care they rely on every day.
“The Harvard Global Health Institute has the ability to spring into action and work across the University to tackle big, new challenges like this,” said Jha. “It’s hard to think of a public health or societal issue that’s more important than the coronavirus pandemic, and we hope this project will help change the national conversation from panic to planning. It’s been remarkable to see the team pull together this important data so quickly. We’ve worked with some of the best journalists in the country so we can make sure people understand what the model is, how to use it, and why looking at the data matters right now.”
A forthcoming HGHI website will allow users to manipulate more factors and test scenarios over longer periods. The researchers are also hoping to incorporate additional datasets, for example on elective surgeries and chronic conditions, to ensure the tool supplies as much high-quality data as possible.