Professor Timothy Rebbeck looks at the reduction in deaths from cancer, the nation’s No. 2 killer.
Kris Snibbe/Harvard Staff Photographer
Drop in cancer deaths lifts U.S. life expectancy
Chan School’s Rebbeck highlights cancer’s complex picture
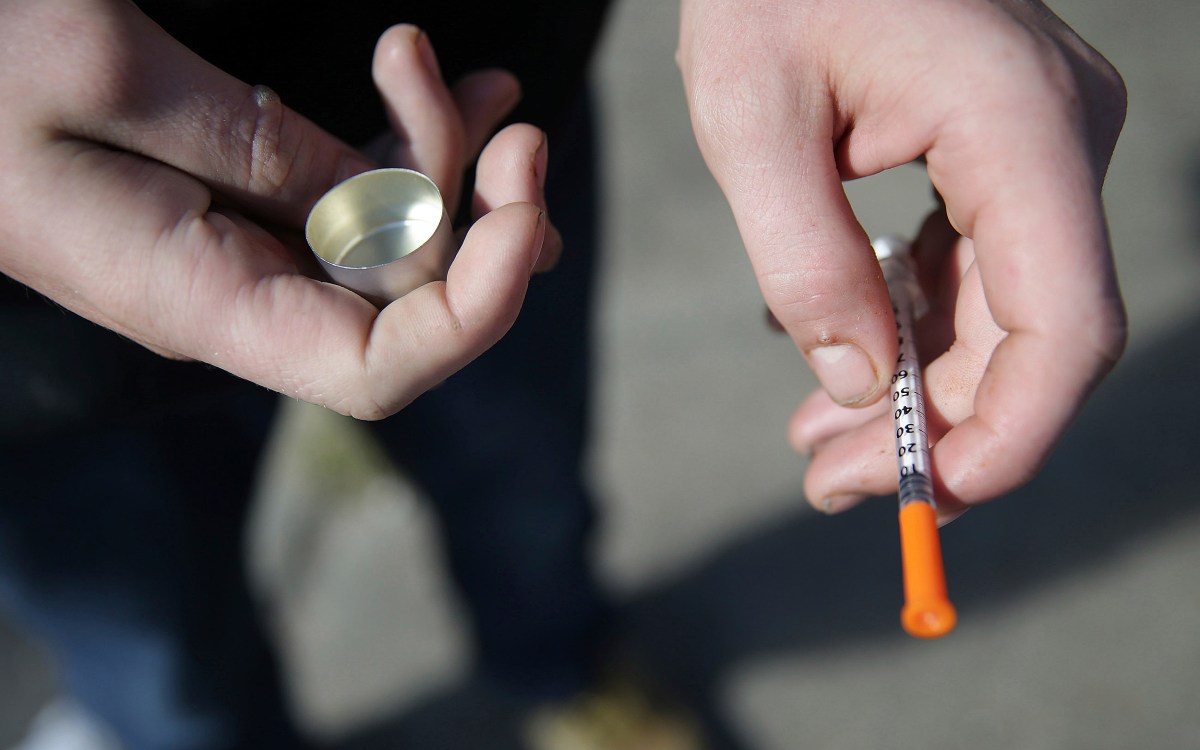
U.S. life expectancy increased in 2018 after a worrisome four-year decline, a reversal owing in part to a welcome decrease in deaths due to overdose but even more so to a drop in those from cancer. The rise brought the anticipated lifespan of someone born in 2018 to 78.7 years, an increase of about a month from 2017 but still short of the 78.9 years reached in 2014. The 2018 figure also included easing in mortality from heart disease and lung disease. The reduction in deaths from cancer, the nation’s No. 2 killer, occurred as rapid advances are being made in treatment with newly developed immunotherapies and precision targeting of tumors’ genetic profiles as well as in detection and prevention. The Gazette spoke to Timothy Rebbeck, the Vincent L. Gregory Jr. Professor of Cancer Prevention at the Harvard T.H. Chan School of Public Health and director of the Zhu Family Center for Global Cancer Prevention, to better understand the good news on the cancer front.
Q&A
Timothy Rebbeck
GAZETTE: The National Center for Health Statistics recently said U.S. life expectancy increased in 2018 for the first time in four years. Part of that was due to a drop in overdose deaths. Getting less attention is that the largest single component of the improving picture was a declining death rate due to cancer. Has that been part of a larger trend?
REBBECK: We’ve seen this trend in cancer deaths over years now. Unfortunately, the decline in cancer deaths hasn’t been as steep as, for example, cardiovascular disease deaths, which have really precipitously dropped over the last few decades. The issue, of course, is that cancer is really a series of diseases, so we see a lot of success in some cancers and less success in others. For example, we see a clear trend in declines in lung cancer and smoking-related cancer deaths because of the decrease in smoking over many decades. There’s about a 20- to 30-year lag before declines in smoking translate into declines in cancer mortality, so we’re seeing this huge decrease in smoking rates pay off in a decline in cancer rates. That’s been happening for a number of years.
GAZETTE: So we’re reaping the benefit of changes from decades ago, at least as far as lung cancer goes. How long will we see these declines?
REBBECK: Lung cancer and smoking-related cancers were almost unknown prior to smoking, so if we can make smoking go away, we can eliminate almost all of the smoking-related cancer incidence and deaths. That’s clearly not happening, but there is a secular trend. The smoking rates in women peaked much later than those in men and declined later, so we expect smoking-related cancer death rates to continue to be a little higher in women than men over a period of time. In another decade or two, we should probably see some leveling of the death rates associated with smoking-related cancers.
“It’s been a miracle of therapeutics that metastatic melanoma is now treatable — and the new approaches were actually discovered at Harvard.”
GAZETTE: Vaping is controversial, in that it’s a potential nicotine-delivery system for the young, but it does offer an off-ramp for people who have difficulty quitting smoking. Do you see that playing an important role in smoking rates and ultimately death rates due to lung cancer in the years to come?
REBBECK: Yes and no. What you said is exactly true. It’s controversial because it’s an on-ramp for teens, but it’s an off-ramp for smokers. Now we’re also learning — there’s been a quite a bit of literature in the past year — that there are plenty of carcinogens, plenty of compounds in the vaping itself that are harmful, so it might not be that vaping itself is all that safe. The carcinogens are not at the same level as cigarette smoke, but it isn’t a completely safe mode of delivery of nicotine, and we don’t really understand exactly how those carcinogens play out in lung cancer or other related cancers, like esophageal cancer. At least right now, vaping is not as common as cigarette smoking, so it’s very hard to predict its impact. Obviously, those of us in public health are concerned that we don’t really understand the risks, which appear to be greater than we thought initially.
GAZETTE: What other cancers are in this picture of increasing life expectancy?
More like this
REBBECK: There are a few in which we’ve seen some really dramatic changes. Some of these are not that common, but they do play a role in the whole picture of cancer-related mortality decline. One is melanoma. Ten or 20 years ago, if you had disseminated, metastatic melanoma, it was essentially a death sentence, and now it’s a quite treatable disease. It’s been a miracle of therapeutics that metastatic melanoma is now treatable — and the new approaches were actually discovered at Harvard. There are cancers like that, where the treatment advances have been really profound, particularly for fatal disease. That has had an impact on mortality, but it hasn’t had a huge impact because the numbers being treated with these agents are still relatively small. But with some cancers, like pancreatic cancer, we haven’t had the same kind of magical therapeutic advances.
GAZETTE: If these therapies are so new that they’re not used broadly, do you expect their impact to increase in years to come?
REBBECK: Yes, and for a couple of reasons. One is that they’re always improving; there are always new things coming along that will treat more people or treat a spectrum of otherwise-resistant disease. The other is that now, not everybody is getting access, there’s a disparity in who is having access. But we hope that as these therapies become more mainstream, more people will get access to them. If this does not happen, the danger is that cancer health disparities may be exacerbated.
GAZETTE: Are racial and ethnic minority groups part of the trend of increased cancer survival?
REBBECK: Definitely for some cancers, but for others it’s either not clear or we know it’s not the case. For example, in breast cancer, both incidence and mortality now are higher in African American women than they are in whites, and that didn’t use to be the case. Many of the benefits of advanced therapeutics, screening, early detection, and genetic testing, haven’t been shared equally in all populations. African American women, for example, have very high rates of breast cancer mortality. That’s happened over years because of the steep decline in mortality of white women, which hasn’t been reflected in black women. So, we see some clear inequities, not just on a patient-by-patient basis but in population-level data. Myeloma is another example, and there are more like that.
GAZETTE: If you were to list cancers that have a good news story versus those that don’t, what would they be?
REBBECK: Metastatic melanoma — advanced disease — is a good example of a success story. Another is cervical cancer, though therapeutics aren’t really the big story there. The big story in cervical cancer is having an HPV [human papilloma virus] vaccination, early detection, and molecular screening that has lowered the rate of advanced disease and therefore death from cervical cancer. We anticipate over the coming decades that in some parts of the U.S., in the U.K., Australia, and other places where they’ve done heavy HPV vaccination and screening, that the death rates from cervical cancer are going to be close to zero. They’ll never completely be zero, but they’re really going to decline. So that’s another success story — a prevention success story. Another example that’s a little different is that of thyroid cancer. Thyroid cancer rates were increasing, but it was being over-diagnosed. Thyroid cancer is common, but a lot of it is indolent. So now they’re getting better, at least in some countries, at knowing how to look for it and those in whom they don’t need to. So the rates of thyroid cancer are dropping because they know they don’t need to look as hard.
GAZETTE: And what about cancers where there hasn’t been much progress?
REBBECK: Mortality rates really continue to be difficult in things like pancreatic cancer and ovarian cancer, even though in some of these cases novel genetic screening exists and, in some people that have high risk, we can intervene earlier and detect tumors earlier. But for many cancers, for people who don’t have these genetic mutations, it’s still quite difficult and therapeutic options, screening and detection options, are still limited. And then there are others like prostate cancer, in which we have a mix. We have really good, new therapeutics in prostate cancer, particularly for advanced disease. And we’re getting a little bit better in understanding who needs treatment and who doesn’t. But we’re really bad at screening for prostate cancer. In 2012, the Preventive Services Task Force and other groups said don’t do PSA [prostate specific antigen] screening anymore. Now, in 2020, we see the rates of aggressive prostate cancer going up, and more men are dying of prostate cancer. So that’s an example where, even though we have better therapeutic options, we’re still really not doing a good job in screening, and as a result, we may see more mortality in the coming years if we can’t get both therapeutics and early detection to work together.
GAZETTE: How much do the improved numbers reflect prevention versus better treatment?
REBBECK: The answer is very much cancer-specific. For cervical cancer, it’s mostly about prevention and in cancers like metastatic melanoma, it’s very much therapeutic. The new therapeutic options like CAR-T cells — immunotherapy — are relatively small but very important and for some diseases a critical advance. But it’s still a relatively small impact on mortality just based on how many people who have these cancers are eligible for those treatments. The big bang for the buck is in prevention and early detection.
GAZETTE: How much do we know about preventing cancer? When you talk about prevention and the work that you do at the Zhu Family Center for Global Cancer Prevention, what are you talking about?
REBBECK: There are a couple of things everybody in the field focuses on, and those are the things that we know work that people aren’t really using. HPV vaccination, smoking cessation, low dose lung cancer screening, colorectal cancer screenings — colonoscopies — are things that we know work, are likely to have a big benefit, but have not really penetrated into the population as much as they should. A second category is new technologies and tools that make early detection and prevention more effective, more efficient, more cost-effective, and more acceptable to patients. There is a huge amount of basic science going on now. Engineers are coming up with technologies and tools and molecular biologists are coming up with things we can leverage to improve early detection and screening. For example, we know a lot about circulating DNA in the blood and if you can identify DNA from a tumor — because it has a mutation or something like that — and you take a blood sample to do a liquid biopsy, you could identify those mutations and say this person is likely to be harboring a tumor somewhere. There are some really cool technologies like that and many others on the horizon that we’re really focusing on, because building on the biology and the basic science, there’s a lot that we can do to make things better.
GAZETTE: Cancer is No. 2 of the top 10 causes of death in the U.S. How long until it drops to No. 3? Or is there a chance that heart disease — No. 1 — is declining fast enough that it will bump cancer up to the top spot?
REBBECK: In Massachusetts right now, cancer is No. 1. Heart disease is below it. There’s a lot of variation in the U.S. Cancer is the leading killer in many places where lifestyle factors have already been improved. So, in a place like Massachusetts, where patterns of diet and exercise and access to health care are better than other places, there’s a lot we can do — and that we are doing — to fight cardiovascular disease. People exercise more, people eat better, people have their cholesterol checked and get to the doctor more regularly. Cancer becomes No. 1 because cardiovascular disease is manageable in many ways and death rates dropped dramatically. For cancer, it’s variable by cancer site and population, and dropping much more slowly. Is it possible that these new therapies will allow cancer to catch up to cardiovascular disease? It’s probably too early to predict, but we would hope so.