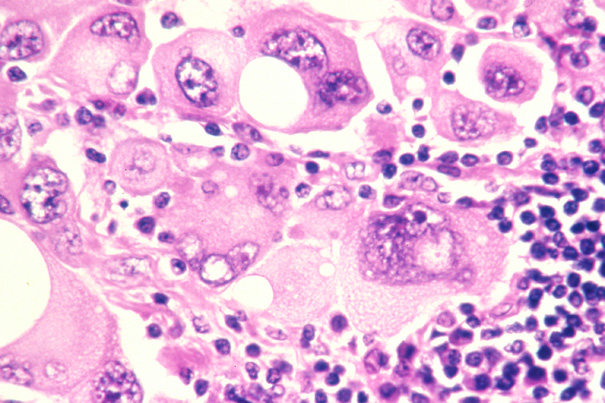
Pictured are human metastatic melanoma cells. A duo of drugs, each targeting a prime survival strategy of tumors, can be safely administered and is potentially more effective than either drug alone for advanced, inoperable melanomas, according to a phase 1 clinical trial led by Harvard investigators at the Dana-Farber Cancer Institute. Image source: Lance Liotta Laboratory
Photo by Sam Ogden
Increasing odds for survival
Combination antibody therapy shows promise in metastatic melanoma
A duo of drugs, each targeting a prime survival strategy of tumors, can be safely administered and is potentially more effective than either drug alone for advanced, inoperable melanomas, according to a phase 1 clinical trial led by Harvard investigators at the Dana-Farber Cancer Institute.
The findings were presented in an oral session at the annual meeting of the American Society of Clinical Oncology on June 4.
The drugs — ipilimumab and bevacizumab — are both monoclonal antibodies, intensified formulations of natural disease-fighting proteins. Ipilimumab spurs the immune system to attack diseased cells, including tumor cells. Bevacizumab, also known by the trade name Avastin, blocks the growth of blood vessels that provide tumors with nourishment. Ipilimumab has extended the lives of metastatic melanoma patients in previous clinical trials, and bevacizumab is often used to treat tumors of the colon, lung, and kidney.
The trial involved 22 patients with metatastic melanoma that was not treatable by surgery.
F. Stephen Hodi, the study’s lead author and director of the melanoma treatment center at Dana-Farber, said the trial is the first to explore whether the two agents enhance each other’s effectiveness. Most of the participants didn’t experience serious adverse side effects, although some did experience inflammation of artery walls, the liver, thyroid gland, colon, or uvea (the middle layer of the eye). Five patients required steroid treatment for these problems and were removed from the trial.
Positron emission tomography (PET) scans showed a prompt immune system response to many of the melanoma tumors, and computed tomography (CT) scans showed decreased blood flow to the tumors. Eight of the participants had partial responses — showing some tumor shrinkage — to the dual treatment, and six had stable disease. All the responses lasted at least six months. Biopsies performed after the treatment showed a more vigorous immune system response than would be expected with ipilimumab alone.
“Our findings indicate that ipilimumab and bevacizumab can be safely administered with careful management of side effects,” said Hodi, who is also an associate professor of medicine at Harvard Medical School. “The results of lab tests suggest that the two agents may work synergistically, with 14 of 21 evaluable patients experiencing a clinical benefit. This approach merits exploration in further clinical trials.”
Funding for the trial was provided by grants from the Melanoma Research Alliance and National Institutes of Health.
The other co-authors of the study are Philip Friedlander, Annick Van den Abbeele, Nageatte Ibrahim, Xinqi Wu, Jun Zhou, Anita Giobbie-Hurder, Travis Hollmann, Sara Russell, Pamela Dipiro, and Jeffrey Yap of Dana-Farber; George Murphy and David McDermott of Brigham and Women’s Hospital; Michael Atkins of Beth Israel Deaconess Medical Center; and Donald Lawrence of Massachusetts General Hospital, all Harvard-affiliated.





