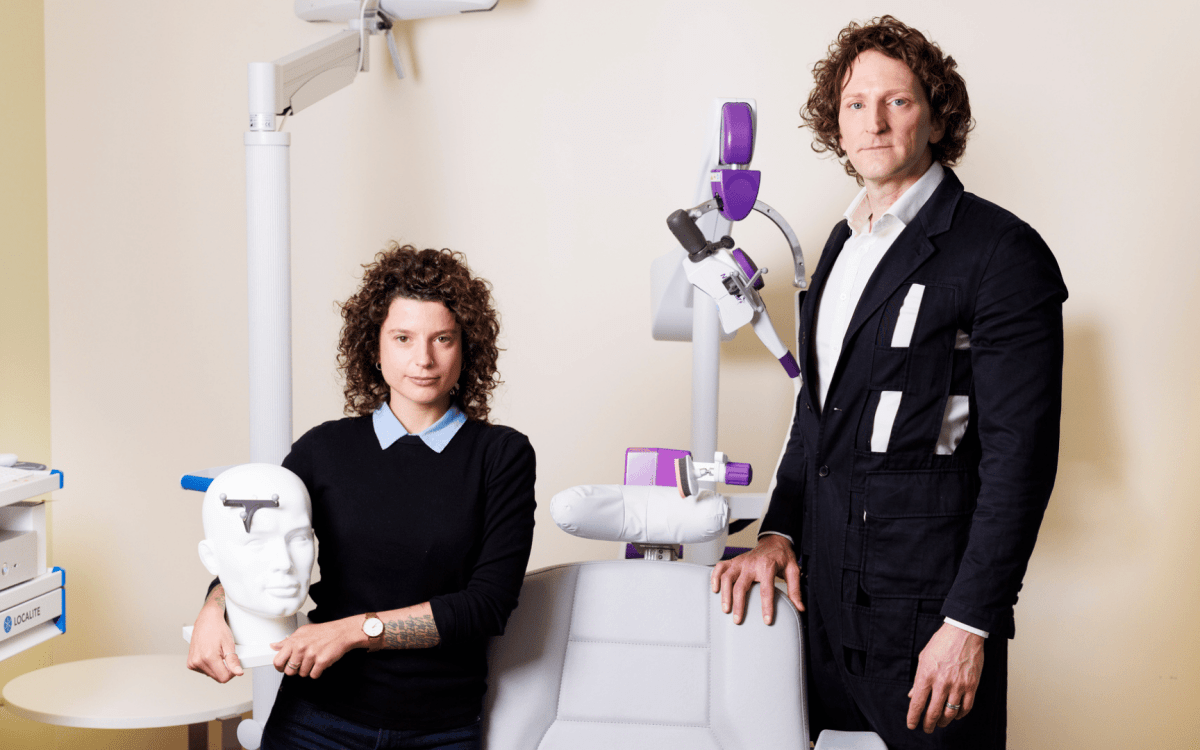
Sobering look at ‘mind-body connection’
Scholar shows religious roots of current practices
Mind-body medicine goes by many names today — including holistic, complementary, or alternative medicine. Regardless of what it’s called, many people embrace the ideas behind the mind-body connection and its effect on health, sometimes despite a lack of supporting scientific evidence.
In her recently published book, “The Cure Within: A History of Mind-Body Medicine” (W.W. Norton and Company, 2008), Anne Harrington explores the long-lived and widespread belief in these unconventional medical practices.
According to Harrington, professor and chair of the Department of the History of Science in the Faculty of Arts and Sciences (FAS), the popularity of mind-body medicine often stems from dissatisfaction with mainstream medicine. Many people with chronic or acute disorders don’t receive satisfactory answers from mainstream or allopathic medicine — or they receive answers that aren’t easy to hear.
“For some,” says Harrington, “the ideas and practices of mind-body medicine — ideas about stress, about positive thinking, about the health benefits of techniques like meditation — help to bring a person’s suffering into focus, help it to make sense, and offer ways for a person to have some perceived direct control over their experience. For these reasons, mind-body medicine can be empowering, and [can] suggest ways that people might change their lives in order to gain control over the course of their disease.”
But as Harrington illustrates in the book, mind-body medicine has an extensive, richly detailed and resonant history, pointing to deeper explanations for why people hold on to these ideas.
One of the reasons for the potency of mind-body medicine, suggests Harrington, is that many of its central ideas have their roots in religion, and particularly in the Judeo-Christian tradition. She cites, for example, the power of suggestion, and applies a psychological interpretation to a healing ritual that goes back to medieval times, when priests exorcized demons, forcing them to leave an unhealthy body. The psychological essence of the ritual persisted, says Harrington, but was first secularized and then medicalized. The result is that today some believe that “authority figures” such as hypnotists can cause symptoms to disappear through the force of an imperative command, much like medieval people believed that priests could cause demons to depart through the power of an imperative.
Similarly, now-secular ideas about the power of positive thinking have their roots, says Harrington, in New Testament accounts of healing through faith. And talk therapy, she adds, which became widely accepted as a treatment for so-called psychosomatic disorders as a result of Freudian psychoanalysis, has its origins in beliefs in the healing power of the ritual of confession.
“Understanding the religious roots of these ideas explains part of their power and why they feel so persuasive,” says Harrington. “These ideas existed as religious narratives before they were scientific or medical narratives. And it seems clear that a religious idea that has been secularized does retain some of the energy that gave it birth.”
The book is structured around what Harrington calls six core narratives that appear repeatedly throughout mind-body medicine and together help us understand why it looks the way it does. These stories address how people believe that the mind has the power to sicken or heal. Each chapter is devoted to one of the six narratives: the power of suggestion; the body that speaks; the power of positive thinking; broken by modern life; healing ties; and eastward journeys.
In the book, Harrington attempts to do justice, she says, not just to the history of the ideas that make up mind-body medicine but to the ways in which these ideas affect people’s personal experiences of illness. She argues, for example, that the history of hypnosis clearly shows that people’s experience of trance states — what happens to their bodies, how they behave — has changed over time in accordance with a changing story about what is “supposed” to happen. Similarly, the experience of stress has also changed: people who lived in cities in the 19th century reported a set of symptoms in response to the challenges of modern life different from the symptoms of today’s urban dwellers. Through this examination, Harrington explains, we see evidence that the experiences of bodies respond to changing cultural cues, and in this way turn out also to have histories of their own.
Within the mainstream medical community today, the mind-body connection is accepted in varying degree. Some deny any effect of the mind on the body beyond the existence of the placebo effect, which they consider to have no lasting therapeutic implications. Others acknowledge the health risks of stress, for example, but are skeptical of more expansive claims for healing through the power of “mind over matter.” Still others consider the placebo effect itself to be evidence of an important mind-body connection based on physiology; are impressed with epidemiological evidence pointing to the health benefits of social support; and point to further evidence for health benefits from other mind-body techniques like biofeedback, hypnosis, and meditation.
The story isn’t over, says Harrington. Historically, some of the ideas of mind-body medicine that were once taken for granted have fallen in and out of favor with mainstream medicine. Harrington points out that it was widely accepted by most physicians until at least the 1970s that diseases such as asthma, ulcers, and even cancer could be caused by repressed emotions and/or stress. Today, few people adhere to that idea in its classical form, and yet variants of these ideas persist on the margins of mainstream medicine. If history is any predictor, it is possible that some of these ideas could re-emerge in some new form in the mainstream.
Even within the medical community, Harrington says, people sometimes respond with regret when an idea from mind-body medicine appears to be scientifically disproved. A recent (December 2007) study looking at the effects of positive attitude on the progress of cancer found that it made no difference. The study resulted in expressions of disappointment by some members of the medical community, and the author of the paper expressed that he was sorry to have to report the results.
We want to believe, says Harrington, in the effectiveness of many of these practices, and we’re attracted to their moral and existential power, even when faced with scientific evidence that should perhaps make us more skeptical.