Rare disease provides cancer detection clues
Breast cancer genes cause other diseases
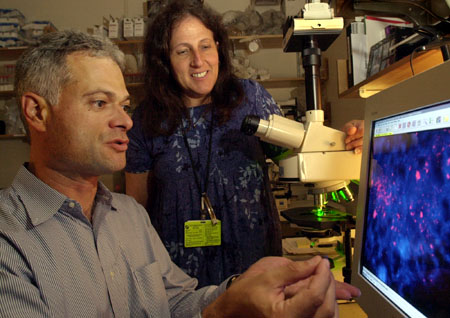
The story began quietly in a small laboratory at the Dana-Farber Cancer Institute in Boston where researchers have been trying to understand a lethal disease of young people called Fanconi anemia. It affects only 500 families in the United States, but Fanconi is horrific. Children are often born without thumbs or other fingers, with small heads, defective kidneys, and abnormal skin color. They lose their ability to make red blood cells, and usually die before age 10 from bleeding and infections. Those who survive with the help of bone marrow transplants (red cells are made in the marrow) die before age 20 from leukemia or other forms of cancer such as malignancies of the head, neck, or esophagus.
Through a series of what they call “eureka moments,” the research team found an association, then a conclusive tie, between mutated Fanconi genes and two genes responsible for most inherited breast cancers.
“In fact, the breast cancer genes themselves can cause Fanconi anemia and all the other cancers suffered by young people with the disease,” says Alan D’Andrea, leader of the team and professor of pediatrics at Harvard Medical School. “As a result, genes once thought to be involved only in breast cancer could provide us with a means for early detection of many different cancers.”
What’s more, Fanconi genes hold the key to producing a promising protein, an enzyme that may lead to a drug that fixes or prevents DNA damage, a problem that underlies both hereditary and nonhereditary cancers.
Confusion leads to discovery
Last year, the Fanconi team, which includes scientists from Oregon, the Netherlands and Japan, found an association between proteins produced by mutated Fanconi genes and by a breast cancer gene known as BRCA1 (see April 19, 2001 Gazette). “You could see them touching each other in the cells of Fanconi patients, but we didn’t know what that meant,” notes D’Andrea, who also holds the title of Ted Williams Senior Investigator at Dana-Farber Cancer Institute.
On a hunch, D’Andrea gave some breast tumor samples to Lisa Moreau, a genetics specialist in his lab. After examining them under a microscope, she announced that the cells came from a person with Fanconi anemia. “It even fooled Lisa, so I knew we were onto something interesting,” recalls D’Andrea
Fanconi and BRCA genes sit on chromosomes, twisted strings of DNA located in the core, or nucleus, of all cells. When treated chemically, the Fanconi chromosomes break up in a distinguished starlike pattern, the same pattern Moreau saw in breast cancer cells.
“Without expecting it, we had discovered a striking visual similarity between the two types of cells,” D’Andrea notes. “That was our first eureka moment.”
“In a way,” he continues, “it made sense. Here was a protein made by the Fanconi gene, which is involved in many cancers, touching a BRCA protein that other researchers had found causes breast cancer. It was guilt by association.”
But more proof was needed. To go beyond what could be seen in a microscope, the researchers sequenced genes from children who had Fanconi anemia but without any mutations of Fanconi genes. These kids are the rarest of the rare; only six to seven families in the United States fit this category. What possibly could be going on, the researchers wondered.
D’Andrea labeled cells from these children “Fanconi anemia” and sent them to Edward Fox, a diagnostics expert at the Dana-Farber Cancer Institute. “We figured there was only about a 1 percent chance that Ed would find BRCA genes in these cells, so the project had a low priority,” D’Andrea recalls. But Fox called him months later, and said the cells must come from patients with breast cancer because he found two mutations of a BRCA gene known as BRCA2.
The conclusion was inescapable. Some Fanconi anemia is caused by mutated breast cancer genes, not mutated Fanconi genes. “It was like closing your eyes, swinging a bat, and hitting a home run,” D’Andrea comments. “It was our second eureka.”
The team had found a new pathway to cancer. If any one of the Fanconi or BRCA genes goes awry, a cell loses some of its ability to repair damage to DNA, damage that arises spontaneously from things such as smoking, X-rays, too much sun, or exposure to certain chemicals. Eventually these errors accumulate and lead to malignancies, which puts everyone at risk for cancer. Those who inherit mutated Fanconi or BRCA genes accumulate such error more rapidly and so develop cancers much earlier.
Double trouble
The discovery is not good news for the parents of Fanconi children, who carry mutations in their breast cancer genes. That puts both the father and mother at a high risk for developing the malignancy. Indeed, many of the parents come from families with strong histories of breast cancer. Recently, D’Andrea had to give them this news at an annual Sunshine Camp, held each year in the United States for Fanconi anemia children from around the world.
“Parents of Fanconi kids spend their lives trying to find a new treatment just to keep the child alive,” D’Andrea points out. “The last thing they need to hear is that they have a high risk of getting breast cancer themselves. That’s another burden they must carry for the rest of their lives.”
D’Andrea now advises these parents to get tested for mutations in their BRCA1 and BRCA2 genes. He also wants to expand these tests to include genes involved in Fanconi anemia because his team has identified a number of families with inherited breast, ovarian and other cancers who have no BRCA mutations. “I expect we’ll find mutations in their Fanconi genes,” he predicts.
In the meantime, such people should avoid substances and habits known to raise cancer risks, such as tobacco, sunburns, and various chemicals and drugs, including those used in hormone replacement therapy. Even mammograms carry some risk of DNA damage and cancer for people with BRCA mutations.
There is some good news in all of this, D’Andrea says. Gene tests will identify some Fanconi family members without an increased risk for cancer, or without the mutations that can cause Fanconi anemia in their children. The researchers also hope that the tragic possibilities will lead drug companies to pay more attention to a disease that, until now, everyone believed affected only 500 families. With the discovery of the connection to breast cancer, new drugs, or those used for other conditions, may help 9,000 people with inherited breast cancer, or even hundreds of thousands with noninherited breast and other cancers.
One possibility lies in healthy Fanconi genes. They produce an enzyme that, along with proteins from nonmutated BRCA genes, plays a role in repairing damage to DNA. Further studies of how this occurs could conceivably lead to ways to strengthen this protective pathway for use against both inheritable and noninheritable breast and other cancers.
“If my lab can contribute to a drug that will strengthen DNA repair and thus delay the onset of cancer,” D’Andrea says, “it will prove my firm belief that understanding rare maladies can provide key insights into much more common diseases.”




