Tag: Harvard Stem Cell Institute
-
Health
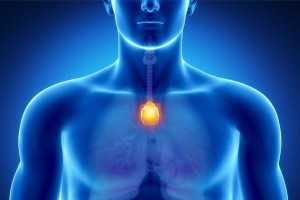
Turns out lowly thymus may be saving your life
Study suggests organ plays vital role in immune health, particularly cancer prevention
-
Health
Breakthrough within reach for diabetes scientist and patients nearest to his heart
One hundred years after the discovery of insulin, replacement therapy represents “a new kind of medicine,” says Douglas Melton, co-director of Harvard Stem Cell Institute.

-
Health
Cells recall the way they were
Study in mice reveals that adult tissues retain a memory of which genes are activated during very early development, and that that memory can be recovered. Under certain conditions, adult cells play their developmental “movie” in a slow rewind, reactivating fetal genes. These findings have important implications for regenerative medicine and cancer research.

-
Health
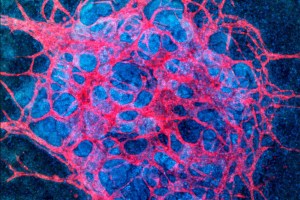
Engineered mini-kidneys come of age
By exposing stem cell-derived kidney organoids to fluidic shear stress, A team of Harvard researchers has significantly expanded the organoids’ vascular networks and improved the maturation of kidney compartments.
-
Health
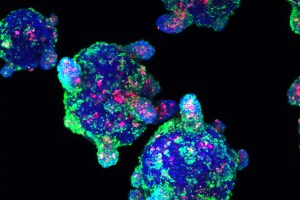
Epidemic of autoimmune diseases calls for action
Scientists at the Harvard Stem Cell Institute are seeking ways to protect newly transplanted cells from autoimmune attack.
-
Health
For new medicines, turn to pioneers
A new study shows that scientific research driven by curiosity is “the best route to the generation of powerful new medicines.”

-
Health
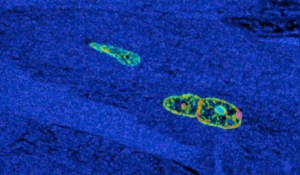
Exercise may help make heart younger
In a new study performed in mice, Harvard researchers found that exercise stimulates the heart to make new muscle cells, both under normal conditions and after a heart attack.
-
Health
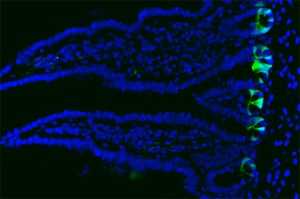
Understanding how the intestine replaces and repairs itself
When working stem cells within the intestine are depleted, some types of mature cells can transform themselves into stem cells, replenishing the population.
-
Health
Study signals need to screen genes for stem cell transplants
Research suggests that genetic sequencing technologies should be used to screen for mutated cells in stem cell cultures, so they can be excluded from scientific experiments and clinical therapies.

-
Health
New vista for brain disorder research
For the first time, researchers describe the types of cells generated in brain organoids, networks of nerve cells, and show the greater diversity, complexity, and response to stimulation developed for nine months and longer.

-
Health
How old can we get? It might be written in stem cells
No clock, no crystal ball, but lots of excitement — and ambition — among Harvard scientists
-
Health
Compound protects nerve cells targeted by diseases
Harvard researchers have identified a compound that helps protect the cells destroyed by spinal muscular atrophy, the most frequent fatal genetic disease of young children.
-
Health
Progress in treating hearing loss
Harvard Stem Cell Institute researchers have developed a drug cocktail that unlocks the potential to regrow inner-ear hair cells, which could help combat hearing loss.
-
Health
How Zika infects the growing brain
Studies have suggested that the Zika virus enters neural progenitor cells by grabbing onto a specific protein called AXL on the cell surface. Now, scientists at the Harvard Stem Cell Institute and Novartis have shown that this is not the only route of infection. The scientists demonstrated that Zika infected neural progenitor cells even when…
-
Health
Colorful clones track stem cells
Harvard Stem Cell Institute researchers have used a colorful cell-labeling technique to track the development of the blood system and trace the lineage of an adult blood cell traveling through the vast networks of veins, arteries, and capillaries back to its parent stem cell in the marrow.

-
Campus & Community
Steven Hyman awarded 2016 Sarnat Prize
The National Institute of Mental Health has awarded Professor Steven Hyman ’80 the 2016 Sarnat Prize for his work on treating and understanding psychiatric disorders as biological diseases.

-
Health
Medical hope on horizon
Stem cell science is accelerating development of therapies for diabetes, ALS, other diseases, researchers tell HUBweek sessions.
-
Campus & Community
Douglas Melton wins Ogawa-Yamanaka Stem Cell Prize
Douglas Melton, co-director of Harvard Stem Cell Institute and the Xander University Professor in Harvard’s Department of Stem Cell and Regenerative Biology, has been awarded the 2016 Ogawa-Yamanaka Stem Cell Prize from the Gladstone Institutes.

-
Campus & Community
Ten from Harvard named HHMI Faculty Scholars
Ten Harvard scientists have won the support of a new funding initiative by the Howard Hughes Medical Institute, the Simons Foundation, and the Gates Foundation.

-
Health
Progress against acute myeloid leukemia
A new drug compound developed by researchers at Massachusetts General Hospital and the Harvard Stem Cell Institute to treat acute myeloid leukemia is gentle enough to use with patients too frail to endure chemotherapy.

-
Campus & Community
At HUBweek, ideas for living
With a wide array of events at the intersection of science, technology, arts, and ethics, HUBweek returns to Boston for a second year. Harvard, one of HUBweek’s founders, will host 14 of the 115 events.

-
Health
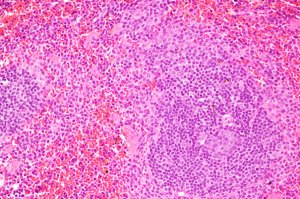
Research suggests new avenues for attacking ALS
Harvard researchers have found evidence that bone marrow transplantation may one day be beneficial to a subset of patients suffering from ALS.
-
Health
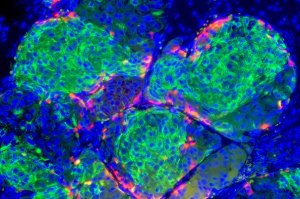
First area cell transplantation center
An expansive effort by several Harvard-affiliated units and hospitals has created the first cell transplantation center in the Boston area.
-
Health
Making bone marrow transplants safer
Harvard Stem Cell Institute scientists have taken the first steps toward developing a treatment that would make bone marrow-blood stem cell transplantation safer.

-
Health
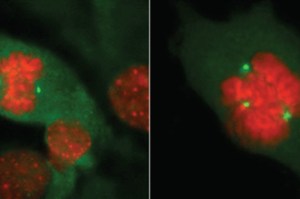
New weapon against breast cancer
Levels of a molecular marker in healthy breast tissue can predict a woman’s risk of getting cancer, according to new research from the Harvard Stem Cell Institute.
-
Health
Alzheimer’s insights in single cells
A study of plaque production at single-cell level holds promise to help improve Alzheimer’s treatment.
-
Health
New drug target for Rett syndrome
Rett syndrome is a relatively common neurodevelopmental disorder, the second most common cause of intellectual disability in girls after Down syndrome. Building on 2004 findings, Harvard researchers identified a faulty signaling pathway that, when corrected in mice, improves the symptoms of Rett syndrome.
-
Health
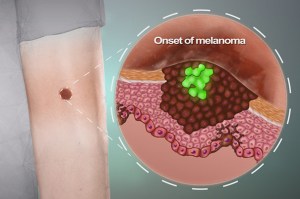
A cancer’s surprise origins, caught in action
Researchers have found that cancer begins after activation of an oncogene or loss of a tumor suppressor, and involves a change that takes a single cell back to a stem cell state. They believe this model may apply not only to melanoma, but to most if not all cancers.